When your ultrasound reveals that your baby’s intestines are developing outside the body, the shock hits hard. You’re staring at the screen, trying to process what the technician just said, and your mind immediately jumps to worst-case scenarios. That’s normal. Most parents in this situation feel a mix of terror, grief, and a desperate need for answers.
The reality is that gastroschisis, while serious, is now highly survivable. More than 90% of babies born with this condition live and thrive. Yes, the road ahead involves hospital stays, surgery, and uncertainty. But with today’s medical care, the majority of children with gastroschisis go on to eat normally, grow, and live full lives. Your baby’s story doesn’t end at diagnosis—it’s actually just beginning.
What Gastroschisis Actually Is
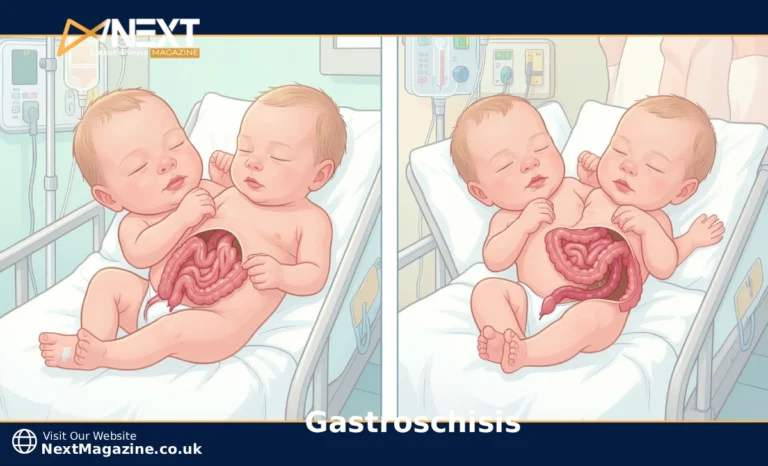
Gastroschisis means your baby’s intestines are protruding through a hole in the abdominal wall, usually right next to the belly button. Unlike some birth defects, there’s no protective sac covering the organs. They’re simply there—exposed, floating in the amniotic fluid throughout pregnancy. When your baby is born, you’ll see the intestines on the outside of the body, and they need immediate specialized care to be safely protected and returned inside.
Sometimes the stomach or liver comes through the opening, too. The intestines might look pink and healthy, or they could appear red and swollen if they’ve been irritated by the amniotic fluid for months of pregnancy. Occasionally, there’s a waxy coating called “peel” on the tissue—that’s just scar tissue from being exposed, and it’s not as alarming as it sounds.
The important thing to understand is that this is a problem with the abdominal wall, not with how your baby’s intestines actually work. Once they’re back inside and healed, most function normally.
Why Gastroschisis Happens
Here’s what every parent wants to know first: you didn’t cause this. Nothing you did or didn’t do during pregnancy caused gastroschisis. This is critical to say because guilt is one of the heaviest emotions parents carry after diagnosis, and it’s undeserved.
The truth is, doctors still don’t fully understand why gastroschisis develops. Somewhere around the fifth to eighth week of pregnancy, the abdominal wall doesn’t form correctly. The muscles that normally close around the organs fail to do so. Researchers have identified some patterns, but nothing definitive enough to blame on parental behavior or lifestyle.
Younger mothers—particularly teenagers and women in their early 20s—have higher rates of gastroschisis than older mothers. After age 25, the risk drops significantly. Some studies suggest smoking, alcohol, or drug use in early pregnancy might increase risk, but many babies with gastroschisis are born to mothers with none of these factors. Environmental exposures, infections, or nutritional gaps have been studied, but no clear cause has emerged.
One thing researchers have noticed is that gastroschisis has become more common worldwide over the past few decades, and no one knows why. This increase has appeared across many countries, which suggests something environmental or lifestyle-related might be involved. But without solid evidence, all we can do is keep investigating and stop blaming parents.
The reality is that gastroschisis happens randomly. It’s not genetic in most cases. You didn’t do anything wrong.
Recognizing Gastroschisis Before and After Birth
Before Your Baby Is Born
The good news is that gastroschisis is almost always caught during routine prenatal ultrasounds. Your technician will see loops of intestine floating freely in the amniotic fluid and will flag it for your doctor. This advance notice, while emotionally difficult, gives you and your medical team crucial time to prepare.
Once you have a prenatal diagnosis, your doctors will monitor your pregnancy more closely. They’re watching for signs that the exposed intestine might be twisted, pinched, or losing blood supply. They’re also checking your baby’s growth and overall development. More frequent ultrasounds become normal, and your anxiety probably increases too—but this monitoring is protective.
At Birth and Beyond
The signs are unmistakable when your baby arrives. You’ll see intestines visibly outside the abdominal area. This moment can be shocking, even though you’ve been told it’s coming. Medical staff will immediately cover the exposed organs with sterile, warm materials to keep them protected and moist. Speed matters here—the first hours of care set the tone for everything that follows.
During those early hours, your baby goes into assessment mode. Surgeons evaluate how much intestine is outside the body, whether it looks healthy, and how easily it might fit back into the abdomen. These details determine what happens next.
The Hospital Journey: What to Actually Expect
The First Days
Your baby won’t eat normally at first. An IV will be placed to provide fluids and nutrition while the medical team prepares for surgery. This is one of the hardest adjustments for parents—you can’t hold your baby skin-to-skin or feed them yourself. You’re watching from the sidelines as professionals do the caring. That feeling of helplessness is real, and it’s one thing hospitals don’t always prepare you for.
During these early days, you’ll meet with neonatologists, pediatric surgeons, and nurses. They’ll explain the surgical plan based on what they see. Your questions might feel endless, and that’s okay. Write them down. Ask them repeatedly if you need to. This is your baby, and you deserve clear answers.
Surgery: Two Main Approaches
Most babies with gastroschisis need surgery within the first hours or days of life. Surgeons choose between two approaches depending on how swollen the intestines are and how much room is in your baby’s abdomen.
Primary closure is the faster option. The surgeon places the intestines back inside the body and closes the hole in one operation. This works best when the intestines aren’t too inflamed, and the abdominal cavity can comfortably hold them. If your baby’s belly is too small or the intestines are very swollen, forcing everything back in at once can put pressure on the lungs and cause breathing problems.
Staged repair takes longer but is gentler. The surgeon places the intestines in a clear plastic pouch called a silo that hangs above your baby. Over several days, gravity slowly eases the intestines back into the abdomen. Each day, the silo is made smaller until everything fits inside. Then the hole is closed in a second surgery a few days later.
When parents first hear about the silo approach, it sounds alarming. But babies tolerate it remarkably well. It looks strange, but it works. Your baby will be more comfortable, and the repair happens safely over time instead of all at once.
Life in the NICU: The Reality No One Mentions
After surgery, your baby enters the neonatal intensive care unit. What follows is weeks—sometimes months—of waiting and watching. Your baby’s intestines need time to “wake up” and remember how to digest food. This takes patience.
You’ll spend hours by the bedside. Some parents camp out in the hospital. Others go home for a few hours of sleep and rush back. You’ll learn machine sounds, tube management, and how to read vital signs on a monitor. You’ll celebrate tiny victories—your baby tolerating their first few drops of breast milk, a successful bowel movement, and being extubated from respiratory support.
You’ll also experience setbacks. Feeds might get held because your baby can’t tolerate them. Infections happen. Your baby might need more surgery than originally planned. The emotional rollercoaster is real, and talking to other NICU parents often helps more than talking to anyone outside that experience.
Nutrition comes through an IV first, then through a feeding tube. Over time, tiny amounts of breast milk or formula are introduced and slowly increased as your baby’s intestines tolerate it. This feeding progression can take weeks. Pain management keeps your baby comfortable during healing, though some discomfort is unavoidable.
The average hospital stay is four to eight weeks, but some babies go home sooner and others stay longer. Every baby’s path is different. Some progress smoothly; others hit complications that extend their time in the hospital. Both are normal.
Long-Term Outlook: Life After Discharge
This is the question that keeps parents awake at night: what happens when we go home, and what does the future actually look like?
Most children who’ve had gastroschisis repair do remarkably well. They eat normally, grow, reach their milestones, and live ordinary lives. Many people have no idea their child was born with their intestines on the outside—because after healing, there’s often no visible sign that anything happened.
Some children face ongoing challenges. Feeding difficulties can persist for months or even years. Some develop oral aversions after being tube-fed for so long, and working with a feeding therapist makes a real difference. Others have trouble with nutrient absorption or deal with chronic constipation or reflux. A small number lose a significant portion of their intestine during surgery and develop short bowel syndrome, which requires long-term management.
Growth delays are common in the first two years. Most children with gastroschisis start smaller than average and gradually catch up. By school age, many are thriving and indistinguishable from their peers.
Surgical scars are permanent, but they fade significantly over time. Some children need additional surgery down the line for scar tissue or hernia repair. These are usually minor procedures compared to the initial repair.
What families mention most is how the NICU experience changes you as a parent. The fear, the uncertainty, the daily ups and downs—it stays with you. Many parents describe feeling intensely protective of their child, but also deeply grateful for ordinary moments other people take for granted. Your perspective shifts permanently, and that’s not necessarily a bad thing.
Parenting Beyond the Hospital
As your child grows, you’ll graduate from the NICU to regular pediatrician care. Some children need ongoing follow-up with pediatric surgeons, gastroenterologists, or nutritionists. Many eventually stop seeing specialists altogether and just see their regular doctor for routine checkups.
Your child will likely have questions about the scar. How you talk about it matters. When children understand their bodies as resilient and strong—not broken or different—they carry that confidence forward. The scar becomes part of their story, not their identity.
Sports, school, friendships, and a normal childhood happen. Your child will probably have times when they notice their scar or remember being hospitalized, but most move forward without letting it define them.
One question parents wrestle with is whether to have more children. The recurrence risk for gastroschisis in subsequent pregnancies is very low—less than 1% in most cases—so it’s safe to have more children if you want them. The decision is usually emotional, not medical. Some families feel ready to try again; others are understandably hesitant. There’s no right answer, and whatever you decide is okay.
Moving Forward
If you’re navigating a gastroschisis diagnosis right now, know that your feelings are valid. Fear, grief, anger, hope—you’ll experience all of them. Take it one day at a time. The path ahead is long, but thousands of families have walked it. They came out the other side, and so will you.
Your medical team will guide you through each step. Neonatal nurses have seen this before and know how to help. Pediatric surgeons specialize in exactly this. And communities of parents who’ve been exactly where you are now exist online and in person—you’re not alone in this.
Your baby’s story is just beginning.
FAQs
Is gastroschisis genetic?
For most families, no. It occurs randomly and isn’t inherited. In rare cases, it can be part of genetic syndromes, but your doctor will discuss genetic testing if other concerns are present.
Can gastroschisis be fixed before birth?
Not currently. Researchers have explored fetal surgery, but it’s not a standard treatment option. Repair happens after your baby is born.
Will my baby eat normally eventually?
Yes. Most babies transition to full oral feeds, though it can take weeks or months. Some need feeding tubes temporarily to help them gain strength before fully breastfeeding or bottle-feeding.
Does gastroschisis affect brain development?
No. Gastroschisis involves only the abdominal wall and intestines. Your baby’s brain develops normally unless there are unrelated complications.
What’s the actual survival rate?
Today, more than 90% of babies with gastroschisis survive, and most thrive. Outcomes have improved dramatically over the past few decades as surgical techniques and NICU care have advanced.
Can you see gastroschisis on ultrasound?
Yes. Prenatal ultrasounds almost always detect gastroschisis. This early detection gives your medical team and family time to prepare mentally and practically for what’s coming.
What’s the difference between gastroschisis and omphalocele?
Both involve organs protruding outside the body, but they’re different conditions. Omphalocele has a protective sac covering the organs; gastroschisis doesn’t. Treatment approaches differ, and your doctor will explain which condition your baby has.